- PATIENT FORMS | REQUEST A CONSULTATION | CONTACT US
- 1-844-NSPC-DOC
A woman with rapid deterioration in vision – Meningioma
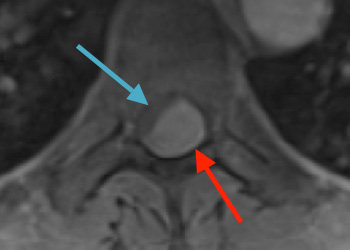
Thoracic Spinal Cord Tumor Case Presentation
October 26, 2021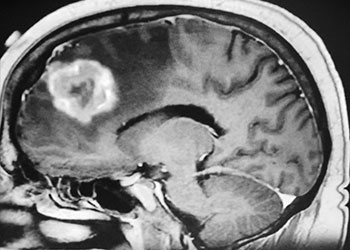
Brain Metastasis
October 26, 2021


Dr. Brisman started the patient on steroids to reduce the surrounding edema. After a few days, the patient did note some improvement in her vision. Due to the size of the tumor, the amount of edema, the rapid progression of symptoms, the patient was scheduled for surgery.
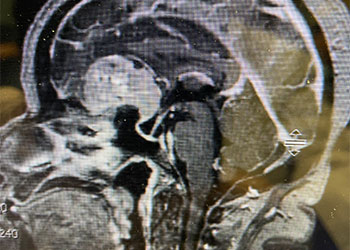
The patient underwent a bifrontal craniotomy and near total removal of the tumor. Because the frontal sinuses were small, it was possible to perform the craniotomy without violating the frontal sinuses. The tumor was removed nearly completely except for a small portion that was stuck to the optic nerves and the anterior communicating artery complex (Figure 2). Postoperatively, the patient immediately noted that her vision had been restored to normal. She was discharged on postoperative day 2. The small remaining tumor will be followed, and may be treated with stereotactic radiosurgery in the future.

Meningiomas can arise from any meningeal tissue within the brain or spinal canal. They are almost all benign tumors. This particular tumor arose from the planum sphenoidale, the flat posterior midline part of the sphenoid bone, a region that forms part of the floor of the anterior cranial fossa. Sometimes these tumors can be removed safely in entirety, depending on how adherent the tumor is to the deep surrounding structures, in particular, the optic nerves, the optic chiasm, and the anterior communicating artery. In this case, the tumor was quite adherent to these most posterior and inferior structures, so it was decided not to risk dissecting this last remaining piece of tumor off these critical structures.
If this tumor were smaller, causing less edema, and no symptoms, it might well have been possible to treat it with stereotactic radiosurgery alone. However, because of the large size, the significant surrounding edema, and the rapid progression of symptoms, it was felt that this was a patient best managed with open surgery. The significant amount of brain edema is expected to completely resolve. The small remaining piece of tumor may be treated at a later date with stereotactic radiosurgery.
CATEGORY: BRAIN // A WOMAN WITH RAPID DETERIORATION IN VISION – MENINGIOMA
A woman with rapid deterioration in vision – Meningioma
This is a 64 year-old woman with no significant past medical history who noted rapid deterioration of vision in her left eye 3 weeks earlier. She said it felt like there was a cloud over her eye. Ophthalmology evaluation confirmed poor vision in the left eye and ordered a brain MRI. The MRI demonstrated a large planum sphenoidale meningioma with significant compression on the optic nerves and optic chiasm and significant surrounding edema (Figures 1 a, b, and c). She was then referred to Dr. Michael Brisman for neurosurgical evaluation.