- PATIENT FORMS | REQUEST A CONSULTATION | CONTACT US
- 1-844-NSPC-DOC
Surgical View of a Microvascular Decompression (MVD) for Trigeminal Neuralgia
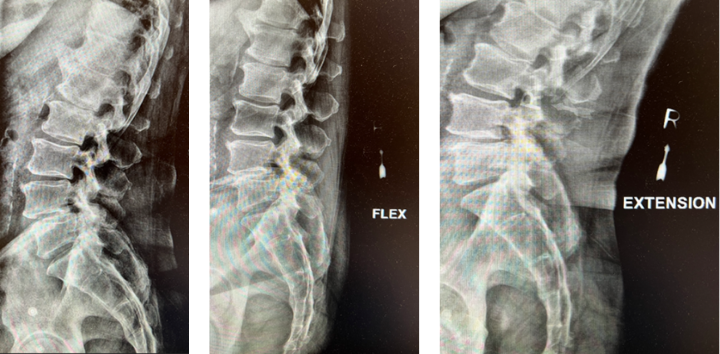
Treatment of Spondylolisthesis and Disc Herniation
May 13, 2022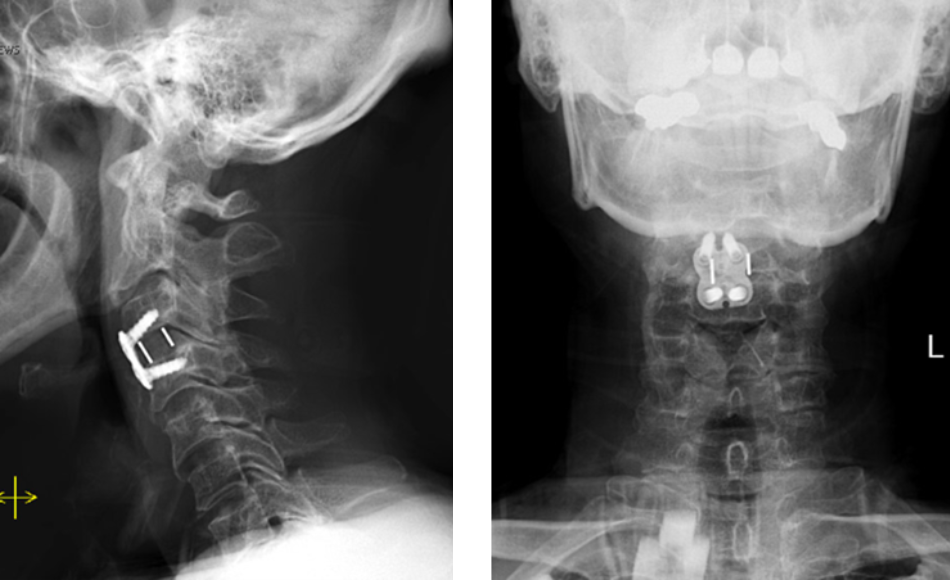
Central Cord Syndrome
June 9, 2022This is a 59-year-old woman with 11 years of left sided facial pain consistent with trigeminal neuralgia. The pain was in her left jaw, cheek and forehead, in all three distributions of the trigeminal nerve. The pains were sudden, brief, severe, electric shocks of pain, that were triggered by light touch and responded to oxcarbazepine. She had tried gabapentin, but that had not been helpful. 10 years earlier she had undergone Gamma Knife treatment which had given her many years of relief, but now the pain had recurred. She had restarted her oxcarbazepine, which gave her partial relief of pain, but caused significant side effects, including dizziness and memory problems. Her prior MRI imaging had demonstrated contact of a blood vessel against the trigeminal nerve root. The patient was healthy other than some medically controlled hypertension and wanted a potentially more permanent procedure to treat her trigeminal neuralgia. As such, she was set up for an MVD.


In my hands, the MVD usually takes about 2 hours once the operation has started. It is performed under general anesthesia, with the patient in the lateral position. Neuro-monitoring is performed throughout the case. A one-and-a-half-inch linear incision is made just behind the ear. A circular piece of bone is drilled out about the size of a quarter (Figure 1). The dura is opened up to the transverse – sigmoid sinus junction, and cerebrospinal fluid is released until the brain is fully relaxed (Figure 2). The microscope is brought in to provide both excellent lighting and magnification. Arachnoid dissection is performed so the vascular conflict against the nerve can be clearly visualized. Sometimes, the endoscope can also be used to clarify the anatomy.


In this case, a loop of the superior cerebellar artery was causing significant compression and distortion of the trigeminal nerve root (Figure 3). The superior cerebellar artery is the usual offending blood vessel in cases of trigeminal neuralgia. Using micro-dissection techniques with appropriate micro -instruments, the artery is dissected off the nerve, and very small pieces of teflon felt (a non-absorbable material) are used to keep the artery from recompressing the nerve. The final image under the microscope shows the trigeminal nerve root fully decompressed, with resumption of normal anatomy (Figure 4).


The dura is closed with permanent sutures (Figure 5). A small round titanium plate is used to reconstruct the skull defect, and the scalp is closed with absorbable sutures. A small sterile dressing is applied (Figure 6). Patients are usually discharged home the following day. This patient did very well. After surgery her pain was completely gone, and she was able to discontinue her oxcarbazepine. Given the surgical findings of a clear and significant vascular conflict, her trigeminal neuralgia pain is likely cured.
CATEGORY: BRAIN // SURGICAL VIEW OF A MICROVASCULAR DECOMPRESSION (MVD) FOR TRIGEMINAL NEURALGIA
Surgical View of a Microvascular Decompression (MVD) for Trigeminal Neuralgia